How do you rule out rabies
Rabies Postexposure Prophylaxis (PEP)
Regardless of the risk for rabies, bite wounds can cause serious injury such as nerve or tendon laceration and infection. Your doctor will determine the best way to care for your wound, and will also consider how to treat the wound for the best possible cosmetic results.
For many types of bite wounds, immediate gentle irrigation with water or a dilute water povidone-iodine solution has been shown to markedly decrease the risk of bacterial infection.
Wound cleansing is especially important in rabies prevention since, in animal studies, thorough wound cleansing alone without other postexposure prophylaxis has been shown to markedly reduce the likelihood of rabies.
You should receive a tetanus shot if you have not been immunized in ten years. Decisions regarding the use of antibiotics, and primary wound closure should be decided together with your doctor.
Rabies
Rabies
What is rabies?
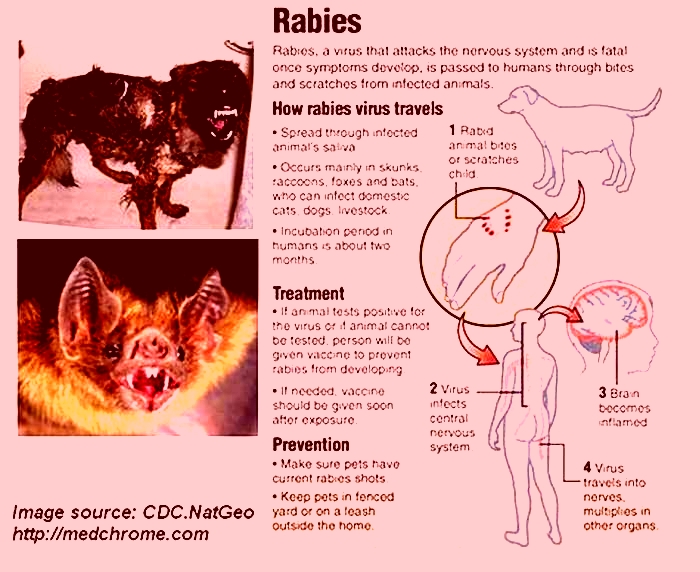
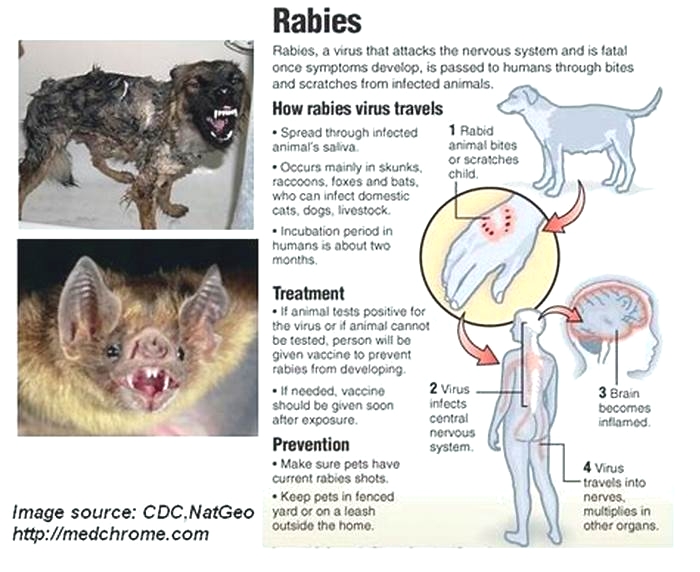
Rabies is a preventable, widespread, viral infection of certain warm-blooded animals. It attacks the nervous system. Once symptoms develop, it's almost always fatal.
In North America, rabies occurs mainly in skunks, raccoons, foxes, coyotes, and bats. In some areas, these wild animals infect pet cats and dogs, and livestock. In the U.S., cats are more likely than dogs to be infected (rabid).
Each state keeps information about animals that may carry rabies. Its best to check for specific information in your local area if you aren't sure about a certain animal and have been bitten. Generally, rabies is rare in small rodents. These include beavers, chipmunks, squirrels, rats, mice, or hamsters. It's also rare in rabbits. The reason for this is that an animal generally has to be attacked by a rabid animal to contract rabies. Smaller animals are less likely to survive this type of attack and go on to develop rabies. In the mid-Atlantic states, rabies is increasing in raccoons. Groundhogs in this area can also be infected.
IIn developing countries, household pets are often not vaccinated against rabies. People traveling to these countries should talk with their healthcare provider about getting the rabies vaccine before their trip.
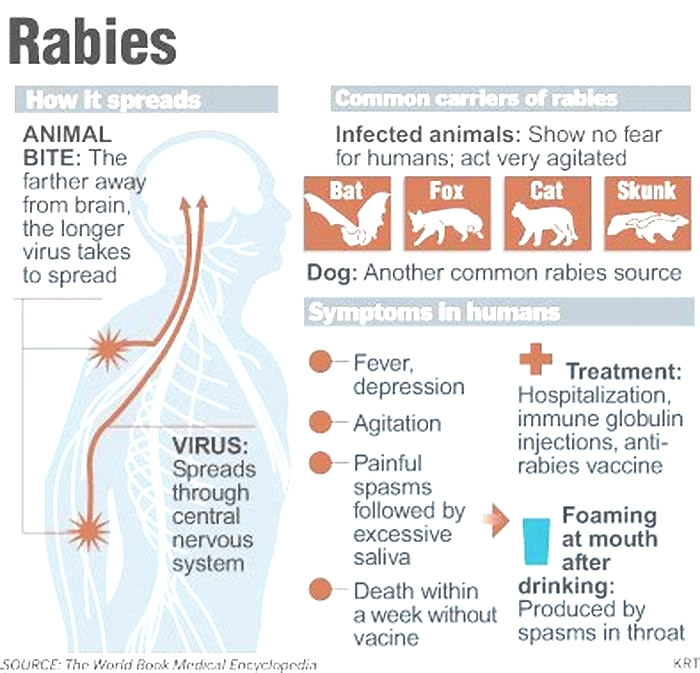
What causes rabies?
The rabies virus enters the body through a cut or scratch. Or it enters through mucous membranes, such as the lining of the mouth and eyes. The virus then travels to the central nervous system. Once the infection is in the brain, the virus travels down the nerves from the brain. It multiplies in different organs.
The salivary glands are most important in spreading rabies from one animal to another. When an infected animal bites another animal, the rabies virus is spread through the infected animal's saliva. Scratches by claws of rabid animals are also dangerous because these animals lick their claws.
Who is at risk for rabies?
Rabies is mainly spread when an infected animal bites a person and exposes them to infected saliva. In rare cases, rabies has been reported from nonbite exposures. These include being exposed in labs when the virus is being handled. Or by breathing in infectious particles in bat caves. In other rare cases, the virus has been spread during an organ or tissue transplant from an infected donor. In the U.S., this risk is reduced because of strict organ and tissue donation guidelines. And because rabies is extremely rare in humans.
Ifa person has been bitten by a rabid animal or exposed to infected tissue or saliva, it is very important to see a healthcare provider right away. The provider will figure out what treatment is needed.
Petting or handling a rabid animal is not considered an exposure. Having contact with infected urine, blood, or stool is also not considered an exposure. Environmental factors, such as temperature and sunlight, affect how fast the virus will become inactive. The rabies virus cant be spread when it dries out and when it is exposed to sunlight. Always contact your healthcare provider to figure out your exposure risk and if treatment is needed.
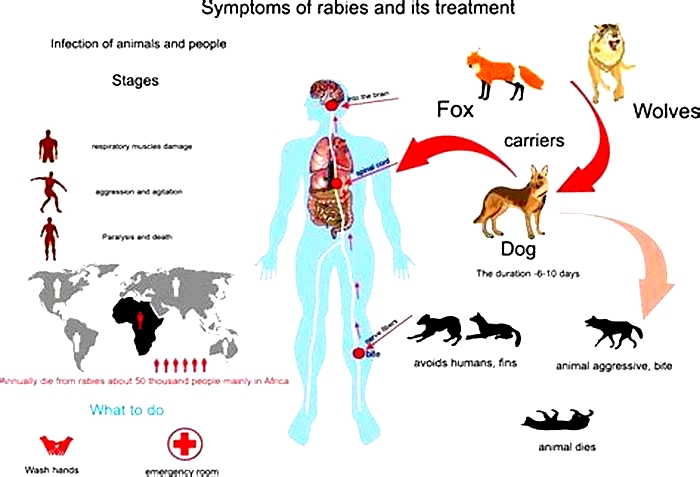
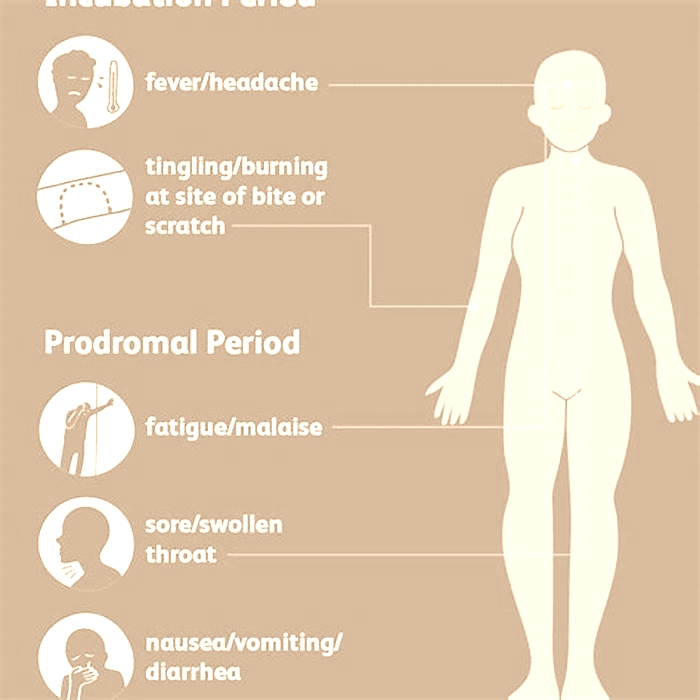
What are the symptoms of rabies?
The time between your exposure to rabies and when the first symptoms appear (incubation period) can range from 5 days to more than a year. But the average is about 2 months. Symptoms may include:
Rabies: Stage 1 | Rabies: Stage 2 |
|---|---|
|
|
The symptoms of rabies may look like other conditions or health problems. Always see your healthcare provider for a diagnosis.
How is rabies diagnosed?
In animals, the direct fluorescent antibody test done on brain tissue is most often used to find rabies. In a few hours, diagnostic labs can figure out if an animal is infected. They provide this information to healthcare professionals. These results may save a person from going through treatment if the animal is not infected. This can only occur if the animal is known or captured.
Several tests are needed to confirm or rule out rabies in people. No single test can be used to rule out the disease for sure. Tests are done on samples of serum, saliva, and spinal fluid. Skin biopsies may also be taken from the back of the neck.
What is the treatment for rabies?
Unfortunately there is no known, effective treatment for rabies once symptoms of the disease appear. But there are effective vaccines that provide immunity to rabies when given soon after an exposure. They may also be used for protection before an exposure happens. They may be used for people such as veterinarians and animal handlers.
If you or someone you know is bitten by an animal, get medical care right away. Remember these facts to report to your healthcare provider:
Where the incident occurred
Type of animal (domestic pet or wild animal)
Type of exposure (cut, scratch, licking of open wound)
Part of the body affected
Number of exposures
If the animal has been immunized against rabies
If the animal is sick or well (if sick, what symptoms the animal had)
If the animal is available for testing or quarantine
The incidents that led up to the bite. Was the bite provoked or unprovoked? Unprovoked bites are more concerning for rabies
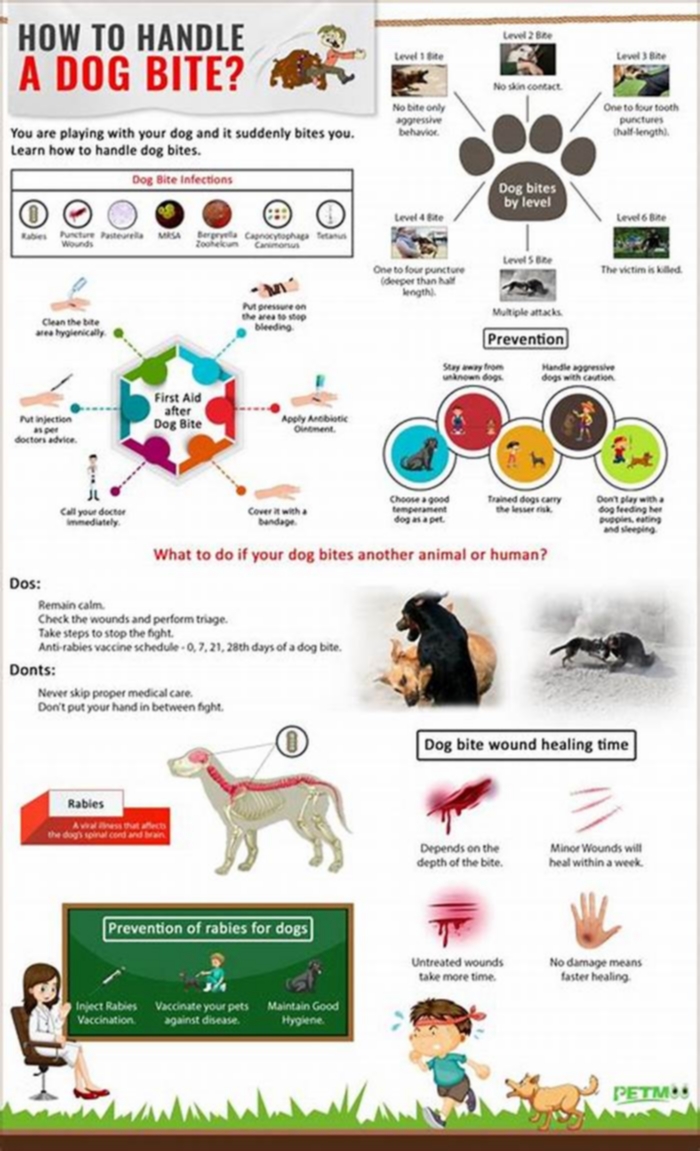
For bites or puncture wounds from any animal, or for any bite from a strange animal:
If the bite or scratch is bleeding, apply pressure to it with a clean bandage or towel to stop the bleeding.
Wash the wound with soap and water under pressure from a faucet for at least 5 minutes. Dont scrub as this may bruise the tissue.
Dry the wound and cover it with a sterile dressing. Dont use tape or butterfly bandages to close the wound. This could trap harmful bacteria in the wound.
Call your healthcare provider right away for guidance in reporting the attack. Also find out if more treatment is needed. This includes antibiotics, a tetanus booster, or rabies vaccine. This is especially important for bites on the face, hands, or feet, or for bites that cause deeper puncture wounds of the skin. It is also important for all cat bites that have a high rate of infection.
If possible, find the animal that caused the wound. Some animals need to be captured, confined, and watched for rabies. Dont try to capture the animal yourself. Contact the nearest animal warden or animal control office in your area.
The affected person may need a series of rabies shots and a dose of rabies immunoglobulin. This may be the case if the animal cant be found or is a high-risk animal (raccoon, skunk, or bat). Or if the animal attack occurred without any cause (was unprovoked).
Call your healthcare provider for any flu-like symptoms following an animal bite. This includes fever, headache, general feeling of discomfort (malaise), decreased appetite, or swollen glands.
What are possible complications of rabies?
Once symptoms of rabies start, rabies most often leads to death.
Can rabies be prevented?
Being safe around animals, even your own pets, can help reduce the risk of rabies. Some general guidelines include the following:
Dont go up to or play with wild animals of any kind. Know that pets may also be infected with the rabies virus.
Watch pets so they dont come into contact with wild animals. Call your local animal control agency to remove any stray animals.
Dont try to separate fighting animals.
Stay away from strange and sick animals.
Leave animals alone when they are eating.
Keep pets on a leash when out in public.
Choose family pets carefully.
Never leave a young child alone with a pet.
Leave all wildlife alone, including injured animals. Teach children to do the same. Contact local animal control officers for assistance. Never touch an injured animal.
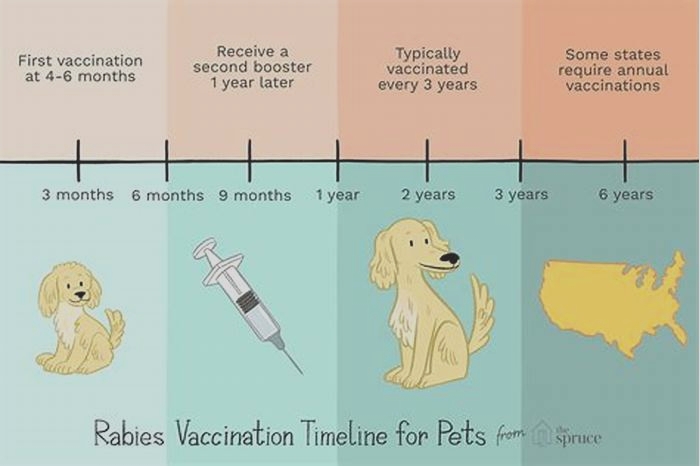
Immunize all pet dogs and cats against rabies and keep shots current.
Make sure your animals wear rabies vaccine tags with the vaccine history, name, and your contact information.
Before traveling to countries where rabies is more common, check with your healthcare provider. Ask about the best strategy for rabies prevention.
When should I call my healthcare provider?
Call your healthcare provider right away if you have any of these:
A bite or scratch from a wild animal that has broken the skin. This might be from a raccoon or skunk.
A bite or scratch from a pet animal that has broken the skin, and you can't be sure that it has had a current rabies vaccine.
You or your child may have been scratched or bitten by a bat. Bites and scratches from bats may not be noticed, especially by children.
Key points about rabies
Rabies is a viral infection of certain warm-blooded animals. It attacks the nervous system. Once symptoms develop, it is fatal.
In North America, rabies occurs mainly in skunks, raccoons, foxes, coyotes, and bats. In some areas, these wild animals infect pet cats and dogs, and livestock.
Rabies is mainly spread when an infected animal bites a person and exposes them to infected saliva.
If you or someone you know is bitten by an animal, get medical care right away.
Several tests are needed to confirm or rule out rabies in people. No single test can be used to rule out the disease for sure.
There is no known, effective treatment for rabies once symptoms of the disease appear. But there are effective vaccines that provide immunity to rabies when given soon after an exposure.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
Know the reason for your visit and what you want to happen.
Before your visit, write down questions you want answered.
Bring someone with you to help you ask questions and remember what your provider tells you.
At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
Ask if your condition can be treated in other ways.
Know why a test or procedure is recommended and what the results could mean.
Know what to expect if you do not take the medicine or have the test or procedure.
If you have a follow-up appointment, write down the date, time, and purpose for that visit.
Know how you can contact your provider if you have questions.
Domestic Animals
Cats, dogs and ferrets
If you were bitten by a cat, dog, or ferret that appeared healthy at the time you were bitten, it can be confined by its owner for 10 days and observed. No anti-rabies prophylaxis is needed. No person in the United States has ever contracted rabies from a dog, cat or ferret held in quarantine for 10 days.
If a dog, cat, or ferret appeared ill at the time it bit you or becomes ill during the 10 day quarantine, it should be evaluated by a veterinarian for signs of rabies and you should seek medical advice about the need for anti-rabies prophylaxis.
| Animal Type | Evaluation and Disposition of Animal | Postexposure Prophylaxis Recommendations |
|---|---|---|
| Dogs, cats, and ferrets | Healthy and available for 10 day observation | Persons should not begin vaccination unless animal develops clinical signs of rabies |
| Rabid or suspected rabid | Immediately vaccinate | |
| Unknown (escaped) | Consult public health officials | |
| Raccoons, skunks, foxes, and most other carnivores; Bats | Regarded as rabid unless animal is proven negative by laboratory test | Consider immediate vaccination |
| Livestock, horses, rodents, rabbits and hares, and other mammals | Consider individually | Consult public health officials. Bites of squirrels, hamsters, guinea pigs, gerbils, chipmunks, rats, mice, other small rodents, rabbits, and hares almost never require rabies postexposure prophylaxis. |
The quarantine period is a precaution against the remote possibility that an animal may appear healthy, but actually be sick with rabies.
The likelihood of rabies in a domestic animal varies by region; hence, the need for postexposure prophylaxis also varies. In the continental United States, rabies among dogs is reported sporadically in states where there is reported rabies in wildlife.
During 2000-2004, more cats than dogs were reported rabid in the United States. The majority of these cases were associated with spillover infection from raccoons in the eastern United States. The large number of rabies-infected cats might be attributed to fewer cat vaccination laws, fewer leash laws, and the roaming habits of cats.
In many developing countries, dogs are the major vector of rabies; exposures to dogs in such countries represent an increased risk of rabies transmission.
Other domestic animals
In all instances of exposure to other domestic animal species, the local or state health department should be consulted before a decision is made to euthanize and test the animal, or initiate postexposure prophylaxis.